AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Elbow humerus fracture12/29/2023  Five patients randomized to ORIF were converted to TER intraoperatively because of extensive comminution and inability to obtain sufficient stability to allow early ROM. They reported that TER resulted in more predictable and improved 2-year functional outcomes compared with ORIF and may result in decreased reoperation rates (12% in TER group vs. conducted a prospective, randomized, controlled trial to compare functional outcomes, complications, and reoperation rates in elderly patients with displaced intra-articular distal humeral fractures treated with ORIF or primary semi-constrained TER. The mean MEPS was 90.5 points, with three patients scoring <75 points. The mean VAS for pain was 0.6, the mean flexion was 123º, and mean loss of extension was 24º. reported 44 TER in treatment of distal humerus fracture patients were followed for a minimum of 10 years. The mean MEPS was 94.3 points, and mean follow-up was 24.9 months. reported seven elderly Asian patients with distal humerus fractures treated with TER and achieved six excellent results and one good result in patients with low physical demands. The complication rate was 9.5% without any revision surgery. reported 21 patients receiving TER for distal humerus fractures with a mean follow-up of 3.2 years, mean MEPS of 84, Q-DASH score of 32.4, mean flexion of 125º, and mean loss of extension of 22º. They reported good or excellent results in 95% of patients at a mean follow-up of 3.3 years, with a reoperation rate of 5%. In 1997, Cobb and Morrey first reported a series of 21 elderly patients who underwent primary TER for comminuted distal humerus fractures. Several studies have reported short- to long-term outcomes and complication rate after TER for complex distal humerus fractures. Radiolucency was graded as type 0 if the radiolucent line was less than 1 mm wide and involved less than 50% of the interface, type 1 if the radiolucent line was at least 1 mm wide and involved less than 50% of the interface, type 2 if the radiolucent line was more than 1 mm wide and involved more than 50% of the interface, type 3 if the radiolucent line was more than 2 mm wide and surrounded the entire interface, and type 4 if there was gross loosening. Implant loosening was graded on anteroposterior and lateral radiographs according to the classification described by Morrey et al. Bushing wear was assessed via anteroposterior radiograph at the final follow-up evaluation and was classified into three grades (normal, mild to moderate, extensive) as described by Ramsey et al. The cementing technique was evaluated on immediate postoperative radiographs for both components and was classified into three types (adequate, marginal, inadequate) as described by Morrey. Serial plain radiographs were performed for all patients to evaluate fixation status, bushing wear, and implant loosening. Clinical outcomes were assessed using the visual analog scale (VAS) score for pain Mayo elbow performance score (MEPS) the Quick Disabilities of the Arm, Shoulder, and Hand (Quick-DASH) score and active range of motion (ROM) of the elbow joint. The mean follow-up period of patients was 29.0 months (range, 12–65 months). These difficulties have led to use of total elbow replacement (TER) as a primary treatment option for complex distal humerus fractures in elderly patients. The complications include fixation failure, nonunion, heterotopic ossification, ulnar neuropathy, and stiffness. The complication rate after ORIF for distal humerus fractures has been reported as over 35%. Successful treatment requires long-term immobilization and produces unsatisfactory clinical outcomes with complications. 
Complex distal humerus fractures in elderly patients may have inadequate internal fixation such that bony union is difficult.  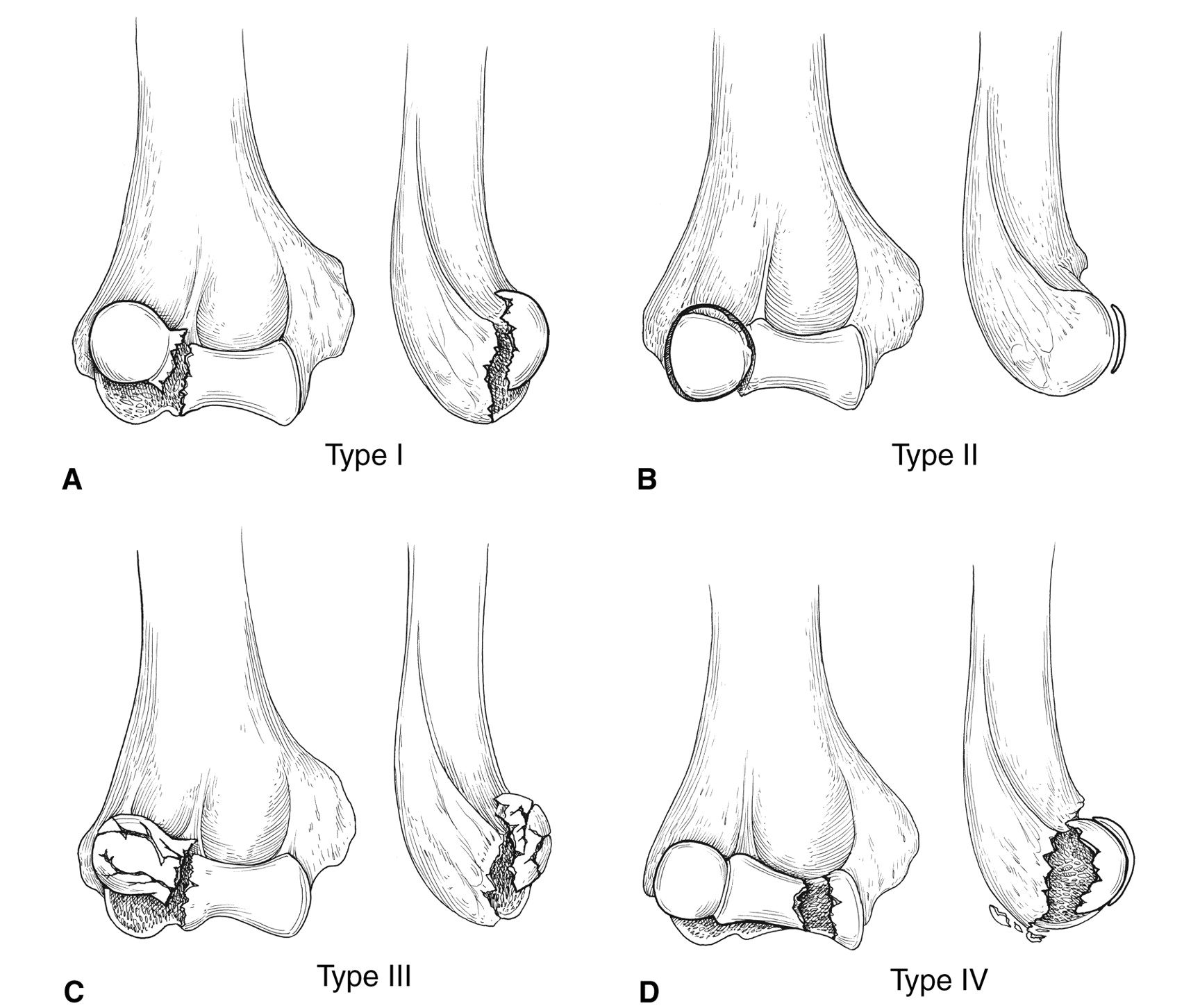
However, these fractures are often complicated by comminution, bone loss, intra-articular involvement, and poor bone quality. 
The gold standard for treatment of displaced distal humerus fractures is open reduction and internal fixation (ORIF), along with early mobilization. Distal humerus fractures in the elderly are increasing with the aging population and are difficult to treat and challenging for orthopedic surgeons. 
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
